
Sep 14, 2022 | EZClaim
As competition in the healthcare industry continues to heat up, providers and billers must look to new options to provide seamless and flexible payment options to retain customers and attract new ones.
Providing a variety of convenient payment options is more important than ever
Patients are frustrated by their healthcare payment options. While they understand the importance of paying their bills, they also want to be able to pay them in a way that is convenient. Many patients would rather pay their bills by credit card rather than cash or check, but they do not always have this option.
Patients have adopted a consumer mindset. From their perspective healthcare transactions should be no different from other transactions. They are more reluctant than ever to put a check in the mail and cross their fingers. In a world of easy online payments and tap-to-pay convenience, healthcare providers need to recognize that the patient financial experience is just as important as the patient care experience.
Most importantly, providing these payment options are not just about giving patients more convenience, but about the bottom line. Embracing new functionality like card-on-file recurring billing and SMS text message payment reminders saves your staff time and increases payment rates.
“We sent out the first SMS payment requests last week, and within several hours had generated 9 payments for a total of over $2,400 back from the patients! The provider is thrilled.”
As the healthcare industry continues to become more competitive, it becomes more critical than ever to create efficiencies wherever possible.
Patient payment data security must be a top priority
In 2016, healthcare organizations suffered a record-breaking number of data breaches. These breaches are not just affecting the health of patients and the financial bottom line of providers – they are also affecting their reputation.
A survey conducted by Ponemon Institute in 2017 revealed that healthcare organizations lost an average of $2.1 million per breach and nearly a third reported losing between $1 million and $10 million per breach. In addition to these costs, there are also significant reputational consequences for healthcare organizations that suffer a data breach. More than half (52%) said they would avoid using a provider following a data breach.
Consumers are concerned about safeguarding their medical information when paying bills; 47% have significant concerns regarding the security of making payments for both medical bills and health plan premiums. They want to take advantage of the consumer protection guarantees that their credit card company offers and a PCI compliant payment processing like EZClaimPay.
Finding the right payment processing partner
Healthcare is more complex than many other industries — a tangle of relationships between patients, healthcare providers, insurers, and unique regulatory requirements such as HIPAA. In this context, there are many providers find that their payment and billing systems do not work well together. Because of these challenges, medical billers and healthcare providers stand to benefit by working closely with their payment processors.
EZClaim set out to build a payment processor from the ground up that addresses these concerns. EZClaimPay helps billers and providers save time and money with functionality like card-on-file recurring billing, ability to offset processing costs with the platform fee functionality, and automatic reconciliation. Plus, increase payment rates with text message reminders and convenient payment portal. Most importantly, because we serve healthcare providers exclusively, we have ensured compliant, industry standard security including PCI compliance.
Streamlining and optimizing payment processing expedites the patient payment process while increasing back-office efficiencies. Healthcare providers that offer seamless, secure, and flexible billing and payment options will retain more customers and continue to attract new ones.
EZClaim is a leading medical billing, scheduling, and payment software provider that combines a best-in-class product with exceptional service and support. For more information, schedule a consultation today, email our experts, or call at 877.650.0904.

Sep 5, 2022 | Partner, Waystar
Switching to Electronic Claim Attachments
One of the biggest strains on the healthcare industry remains its reliance on paper and manual processes. The combination often adds up to human errors and costly denials, which require exponentially more time and resources to resolve, if left unchecked.
Among the manual processes most challenging to manage is claim attachments, which demand considerable time for teams to review requirements, collect and send necessary documentation, and complete follow-up procedures. According to the CAQH Index, the medical industry spent $590M annually exchanging attachments, with some providers spending anywhere between 10-30 minutes manually submitting an attachment to a payer.
An electronic claim attachments solution bolsters efficiency, strengthens cash flow, and significantly reduces AR days. If you’re considering how such a solution could benefit your healthcare organization, read on to learn about three key areas it can improve.
- Simplify document + data exchange with payers
Despite technological advancements, providers still face a complex, manual environment for payer document and data exchange. Electronic claim attachments can help ease long-standing friction points between providers and payers by automating supporting documentation submission. It’s a win-win for providers and payers as workflow efficiency can be maximized and claims adjudicated more swiftly and correctly.
- Support frictionless and remote workflow
Processing claim attachments becomes exponentially more time-consuming and expensive because of its paper-based nature and the need to keep up with ever-changing payer rules and requirements. Shifting to electronic claim attachments can provide flexibility to ensure your billing team can continue to operate effectively even in disruptive times. It not only saves time and money each day but it’s also proved critical during events like Covid-19, allowing a divided workforce to still get the job done.
- Reduce cost to collect
Not all clearinghouses are created equal—the right partner fervently seeks opportunities for staff to work smarter, not harder. Automation and scale are key elements to not only maximize efficiency and accuracy but also reduce a provider’s cost to collect.
Although electronic attachment adoption remains low, there’s considerable benefit to implementation. While electronic transaction for claim attachments has not yet been federally mandated, the 2020 CAQH Index found the medical industry could save over $377M per year, helping organizations protect their bottom lines and provide more affordable care to their patients and communities.
Wrapping it up: taking the smarter approach to submitting attachments
Providers are all under cost and reimbursement pressure and the need for smarter, purpose-built automation is the secret ingredient for remaining in the black. Electronic claim attachments are a simple way to take the administrative waste out of your processes, prevent costly denials and accelerate cash flow, all the while supporting a remote workforce.
Looking for a smarter, simpler way to manage claim attachments and streamline workflows? Find out how Waystar can help automate the process, reduce denials and accelerate reimbursement. Visit Waystar.com.
ABOUT EZCLAIM:
As a medical billing expert, EZClaim can help the medical practice improve its revenues since it is a medical billing and scheduling software company. EZClaim provides a best-in-class product, with correspondingly exceptional service and support. Combined, EZClaim helps improve medical billing revenues. To learn more, visit EZClaim’s website, email them, or call them today at 877.650.0904.

Aug 11, 2022 | EZClaim
The revenue cycle is a crucial component of a medical practice. Revenue Cycle Management (RCM) is the process of managing patient accounts, interacting with payers, processing claims, and collecting payments related to health care services. As the industry becomes more competitive and physicians are expected to perform more administrative tasks on their own, RCM has become even more important for healthcare providers today than ever before. Unfortunately, many practices still struggle with managing their RCM processes in an efficient manner that allows them to focus on what matters most: patient care. Below is a list of common mistakes made by healthcare providers when it comes to RCM.
Below is an overview of the seven key components of RCM and ways to avoid some of the most common mistakes.
Insurance Verification and Authorization
Insurance verification and authorization is a critical step in the revenue cycle process. If this step fails, all other steps must be repeated. This can result in delays, rework, denials of claims and even patient non-compliance.
- Verify that the patient is covered by their insurance plan and will not be responsible for additional costs related to their treatment or procedure (co-pay and deductibles).
- Verify that your provider is in network for each specific procedure with their chosen health plan/policy before completing any work on behalf of the patient.
- Ensure that all documentation supports your claim(s), including diagnosis codes and clinical notes from EMRs or doctors’ offices detailing what was performed during each visit. These details should align with those found on physical charts signed by both patients and providers alike.
- Verify eligibility rules as defined by health plans: has a deductible been met? Is there a copay amount due before benefits kick in? In some cases it may be necessary to contact members directly via phone or email asking them these questions so they know exactly how much they owe out-of-pocket. Our partner TriZetto Provider Solutions offers integrated eligibility verification. Automating this due diligence on the front end ensures that you are not left with the cost of having a biller redo this work, or worse, writing of claims.
Patient Registration and Copay Collection
Patient registration and copay collection are important first steps to ensure that your revenue cycle is functioning properly. Patient service, claims submission, remittance processing, and back-end patient collections are all vital components of the revenue cycle management process.
Without these steps in place, you will not be able to complete the full revenue cycle management process.
Service Coding and Charges
The service coding process identifies the type of service or procedure that was performed by your staff. Accurately documenting and coding charges allow you to:
- Assign appropriate codes for reimbursements from government programs, insurance companies and self-pay patients.
- Determine the level of reimbursement for each code
- Avoid fraud and abuse
Billing and Collections
It is critical to collect payments on time, in full and accurately. If you do so consistently, it will be easier to predict future cash flow needs and improve your ability to manage the revenue cycle.
Timely billing is critical because it allows the practice to collect their fees before they become delinquent. Delinquent accounts must be reported to credit agencies which can negatively impact a patient’s ability and willingness to pay for other services at your facility in the future. Late fees should also be considered for patients who are more than 60 days late paying their bill – this can help generate additional revenue by encouraging prompt payment from patients who may otherwise have ignored their bills altogether.
Accuracy is key when collecting payments because inaccurate claims may result in denied reimbursement by Medicare or third-party payers’ due out-of-pocket expenses for patients who were mistakenly overcharged by providers.
Consistency means that providers need regular updates on where each account stands within its cycle; this helps ensure that both patient satisfaction levels remain high and that everyone receives timely access. Efficiency refers not only to how quickly accounts move through management but also how quickly they get paid so providers know exactly how much money they’ll have coming in each month before making subsequent budgeting decisions.
EZClaim provides great tools to help ensure your collections are timely, accurate, and consistent. EZClaim allows you to keep a credit card on file. With approval to charge up to a specified amount, you can make it convenient for your patients and ensure payments are timelier than ever. EZClaimPay also offers email and SMS text message-based reminders, which have proven effective in increasing payment rates.
Denial Management
Denial management is the process of managing patient denials. Denials can be caused by a variety of reasons, including incorrect CPT codes, missing information, or provider errors. Therefore, it’s important to have ready-to-go processes for handling them and getting paid as soon as possible.
When you receive a denial from an insurance company, there are several things you should do immediately:
- Double-check that all your claims are accurate and complete before submitting them for payment. If there is any ambiguity on the part of the patient or their healthcare provider, this will increase the likelihood that your claim will be denied due to lack of clarity.
- Request that more specific details regarding the denial be provided. This allows better preparation when submitting future claims related to this patient’s care and ensures there aren’t additional denials for similar reasons.
The revenue cycle is a crucial component of any medical practice. It’s also one of the most challenging aspects of running a practice, especially in today’s increasingly complex environment. This article has highlighted some common mistakes that can be made when managing your revenue cycle and how to avoid them.

Jul 19, 2022 | EZClaim
Demand for different care models and emerging technologies are changing how healthcare is delivered in 2022. These are the trends to watch this year.
More Medical Technology Integration
Integrating medical technologies to broaden available data and improve patient outcomes will continue to impact the way hospitals, healthcare centers, and care providers operate. These new tools and integrations will allow healthcare professionals to use more efficient workflows thanks to better APIs and less data silos.
Integration means collecting more data with new remote monitoring and Medical “Internet of Things” devices. This data can then be centralized for patients and doctors with with cloud-based electronic health record platforms. It also means better patient education with consumer mobile apps, automated care-team emails and text messages, and digital therapeutics. These integrated tools will continue making it easier for doctors to collect and access more precise and detailed patient data than ever before.
As more technology works together, providers can identify and solve medical issues faster and more accurately. Further, patients are given opportunities to become more involved in achieving their healthcare goals and taking part in preventative measures.
Telehealth Continues to Grow
Today, many providers offer telehealth options to patients who prefer to meet with their doctor via phone or video. This option is one of the fastest growing in healthcare and will be an increasingly popular way to access healthcare in the coming years.
Telehealth can be beneficial for both providers and patients by lowering costs and increasing availability. Telemedicine allows healthcare providers to reduce their overhead and pass on those savings to patients by removing the need to visit a physical office. In addition, telehealth capabilities have made rural access easier by giving Americans a broader range of providers in different specialties. Traveling for healthcare can be expensive in terms of money and time. Virtual care offers lower costs, greater access to primary care for those in rural areas, and better public health.
The option to meet with a provider by phone or video is also a great tool to bring in and retain new patients. Lowering barriers to entry and establishing relationships via video or phone can be a great way to provide quality care initially and preserve that patient over the long term.
Healthcare consumerism was slowly growing before COVID, and patients see technology as a way to improve their mental and physical well-being. Telehealth will play a major role in those consumer expectations.
Home Health will Become More Popular
As more baby-boomers hit retirement age, demand for home health nurses and services—which were already seeing a surge in demand with COVID-19—will only continue to increase. As home health monitoring technology becomes increasingly available, states and private equity increases funding for these programs, and many seniors opt to return home instead of a skilled nursing facility, the trend towards home health is clear.
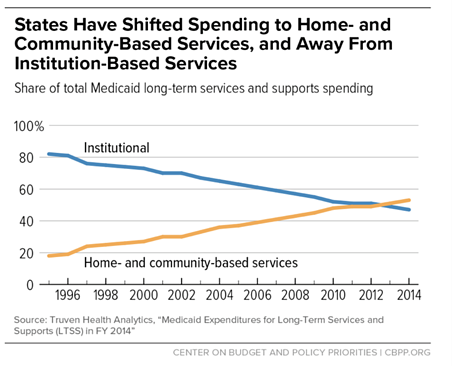
Medicare data reflects this trend as well with the Medicaid Innovation Accelerate Program reporting continued growth in home and community services.
Emerging technologies and care models are driving the way forward in 2022. These innovations will provide new ways for providers to deliver better care and more value to their patients.
EZClaim is a leading medical billing, scheduling, and payment software provider that combines a best-in-class product with exceptional service and support. For more information, schedule a consultation today, email our experts, or call at 877.650.0904.

Jun 17, 2022 | Partner, Trizetto Partner Solutions
We already know the trend toward automation in healthcare continues to grow each year. As technology continuously improves and the financial bar to entry lowers, the opportunities for healthcare providers and health plans to enhance operational processes grow as well. But even with the radical progress and the easier-to-use-than-ever healthcare operations software, many organizations fail to implement the solutions. It may be a lack of organizational enthusiasm or a simple need for more skilled internal technological expertise.
And while this is likely common knowledge at your organization, the amount of money wasted each year – driven by the absence of process automation – may not. Billions of dollars that could otherwise be spent on improving patient care and satisfaction, on building and rolling out new service lines, and generally improving healthcare operations are wasted every year. Billions.
The most recent CAQH Index reports $372 billion is spent yearly on administrative tasks throughout the US healthcare system. Of that amount, $39 billion of those administrative transactions are specifically tracked by the CAQH Index. “Of the $39 billion, the industry can save $16.3 billion, or 42 percent of existing annual spend, by transitioning to fully electronic transactions,” according to CAQH.
$16 billion in savings.
The current opportunity for savings driven by automated, electronic transactions within the healthcare industry is tremendous. That’s not to say the healthcare industry is doing nothing. CAQH found that healthcare organizations already save $122 billion annually thanks to process automation.
Even with the apparent success of automation, however, CAQH found the utilization, adoption, and growth of fully-automated processes year-over-year was stagnant or modest at best:
-
-
- Eligibility and benefit verification remained steady at 84%
- Prior authorizations increased to 21% from 13%
- Claim status inquiry grew slightly to 72% from 70%
- Claim payment automation increased marginally to 71% to 70%
With the small and slow shift to the use of automated transaction processes in the healthcare industry, there’s a decided advantage–in time and money–to not automating many, if not all, backend operations. Doing so allows staff to focus on strategic initiatives, like building out new programs or service lines, rather than plodding through everyday tasks better tackled through repeatable processes supported by technology.
“The industry continues to make progress towards a more automated administrative workflow as transaction volume increases, new business needs and technology emerge, and health insurance benefit and payment models evolve,” CAQH explains in the report. Nevertheless, as mentioned earlier, the “progress” remains slow, like a river choked with debris.
Ironically, even as automated solutions become more abundant and easier to use, CAQH reports healthcare providers to perform more manual tasks today than in the past. With today’s technology-rich environment, there’s little reason for healthcare providers to input any type of care-related documentation by hand. That time can and should be better spent improving the healthcare experience for patients and their families.
It’s far past time to clear the detritus from the river. With the advantage of today’s technology, it’s easier to make the change when each of us plays a part in the cleanup.
Contact a TriZetto Provider Solutions representative today to learn more about automation-enabled technologies that can help drive efficiencies and increase revenue.
EZClaim is a leading medical billing and scheduling software provider that combines a best-in-class product with exceptional service and support. For more information, schedule a consultation today, email our experts, or call at 877.650.0904.
[ Contribution from the marketing team at TriZetto ]







