
Feb 9, 2021 | Claim Status Inquiry, Claims, Denied Claims, Electronic Billing, Medical Billing Software Blog, Partner, Waystar
Reducing claim denials has long been a challenge for providers. In the worst case, denied claims end up as unexpected—and sometimes unaffordable—bills for patients. The challenge only seems to be growing. A recent survey conducted by the American Hospital Association (AHA) found that 89% of respondents had seen a noticeable increase in denials over the past three years, with 51% describing the increase as “significant.”
Minimizing loss will be top of mind for providers as the COVID-19 pandemic continues to put a strain on their resources, and minimizing or preventing denials will need to be a core part of that strategy. With that in mind, we’re offering four tips to help guide revenue cycle strategies for better denial reduction in 2021.
1. Analyze and Assess
In order to achieve and maintain a healthier denial rate, it’s vital to have a good handle on the factors creating problems in the first place. Keep the following in mind as you start to structure your analysis:
- Review key performance indicators: Take a look at which metrics are being used to benchmark success or failure and see if it’s time for a refresh
- Evaluate workflows: It’s important to have a clear understanding of how your team operates, and that you can detail workflows as step-by-step processes
- Assess tools: Inventory the software you’re using and discuss with your team how it helps or hinders them
- Staff efficiency: Consider the number of team members and resources involved in each step of the denial management process
It’s also important to talk to staff. Your team can offer invaluable insight on what is and isn’t working to help you develop a more comprehensive understanding of the shape and scope of the systemic issues contributing to your denial rate.
2. Reduce Errors Upfront
Eligibility, registration, and authorization errors remain the greatest cause of denials and write-offs, so a good first step is to focus on being proactive instead of reactive. Often, it’s easy to get into a routine where errors are only addressed after they occur. But incorporating tech to verify coverage and benefit accuracy in advance can lead to higher efficiency and much less manual labor spent to correct those issues later on.
Similarly, a recent AHA report found a failure to obtain prior authorization to be one of the most common reasons for a claim to be denied by a commercial health plan. In another recent survey, the American Medical Association found that 86% of providers surveyed were struggling with a high administrative burden created by prior authorizations.
Recent innovations have made the process simpler than ever. The right prior authorization solution can automate the process and make it simpler, smarter, and much less labor-intensive, reducing manual input errors and preventing denials.
3. Cut Down on Manual Labor
Claim denials are often the result of staff trying to keep track of a seemingly overwhelming number of rules and regulations while juggling various systems and filing requirements. When your staff is overburdened, it’s that much easier for them to make simple errors or miss deadlines.
There are numerous tools available for teams who are either struggling with paper-based processes or databases without automation. With an AI-powered solution, you can streamline a number of time-consuming tasks while simultaneously automatically ensuring you’re identifying missing data or claim errors that can be corrected before they’re submitted.
It’s also a good idea to review any potential new tools with your team. Their insight will help you properly determine which solutions will actually improve their workflows, and which could prove an expensive time sink.
4. Use Stronger Reporting Tools
Accurate and in-depth reporting should be core to your strategy. Effective reporting tools let you quantify and assess the issues that influence your denial rate, allowing you to easily spot persistent workflow errors or other systemic problems that can create extra work or strain resources.
New tools powered by AI and machine learning offer more robust reporting options than ever, with advanced analytics and visualization capabilities that make it easy to explore complex data sets or identify trends. Mountains of information can now be easily managed and measured, giving you access to operational insights that will help you better understand problem areas and identify opportunities for improvement.
The Wrap-up
With the right tools, a solid strategy, and expert guidance, you can take a proactive approach to reducing claim denials. Our automated tools make it easy for your team to streamline their workflows while reducing errors and administrative costs. With Hubble, our AI and RPA platform, you can unlock the insights you need to reduce your denial rate and increase cash flow.
Waystar, a partner of EZClaim, also offers a number of front-end solutions to help you take a more proactive approach to your denial rate. Click here to learn more about how Waystar can help you with reducing claim denials and claim management. For more information about Waystar’s platform, visit their website, or give them a call at 844.492.9782.
To find out more about EZClaim’s medical billing software, visit their website, e-mail their support team, or call them at 877.650-0904.
[ Contribution: Waystar ]

Nov 10, 2020 | Medical Billing Software Blog, Partner, Trizetto Partner Solutions
To adjust to the ‘new normal’, here are some of the latest best practices for medical offices to implement.
In the current state of the world, filled with struggles brought on by COVID-19, many providers and practices are attempting to weave new procedures and workflows into their daily activities—to adjust to the ‘new normal’. This includes implementing virtual visits, exploring automation and paperless options, streamlining eligibility verifications, and strategizing on denials management.
An EZClaim partner, TriZetto Provider Solutions, has provided information about the latest best practices for medical offices. Their in-house experts offer some creative ways of how your practice can become more efficient and navigate through the pandemic with the following articles:
• Eligibility Woes: The Impact of COVID-19 on Insurance Coverage
• Adapting denials management to protect and retain revenue
• Healthcare Huddle: How to Manage Telemedicine & New Challenges during the New Normal
EZClaim’s medical billing software can ensure that you are equipped with the right solutions to manage costs and maximize revenue flow. Want to learn more? Well, visit their website, e-mail them at sales@ezclaim.com, or call a representative today at 877.650.0904.

Sep 10, 2020 | AMBA National Conference, Medical Billing Software Blog, Support and Training
EZClaim is always looking for ways to help our medical billing clients improve. In an effort to further that mission, this month we are kicking off the first in a series called, “What’s Current in Coding.” In this series, we will highlight coding topics, events, webinars, and more, all with the aim of keeping you current in medical billing and coding.
This month our focus came from two articles on coding sourced from the AMBA Newsletter that we feel are hot topics of the industry: “Coding for Group Visits” and the “Telehealth Coding Guide.”
Below you will find full articles and source links.
ARTICLE 1: “Coding for Group Visits”
Many physicians are interested in providing group medical visits. Whether the drop-in group medical appointment (DIGMA), chronic care health clinic (CCHC) or other model is delivered, the coding and billing of these services raise questions about codes and payment policies.
While past instruction on coding for group visits often indicated that physicians should report code 99499 for unlisted evaluation and management services, using this code requires that documentation is sent with the claim to identify the service(s) provided and leaves valuing of the service in the hands of the payer.
No official payment or coding rules have been published by Medicare. However, the question of “the most appropriate CPT code to submit when billing for a documented face-to-face evaluation and management (E/M) service performed in the course of a shared medical appointment, the context of which is educational”, was sent to the Centers for Medicare and Medicaid Services (CMS) with a request for an official response. The request further clarified, “In other words, is Medicare payment for CPT code 99213, or other similar evaluation and management codes, dependent upon the service being provided in a private exam room or can these codes be billed if the identical service is provided in front of other patients in the course of a shared medical appointment?”
The response from CMS was, “…under existing CPT codes and Medicare rules, a physician could furnish a medically necessary face-to-face E/M visit (CPT code 99213 or similar code depending on level of complexity) to a patient that is observed by other patients. From a payment perspective, there is no prohibition on group members observing while a physician provides a service to another beneficiary.” The letter went on to state that any activities of the group (including group counseling activities) should not impact the level of code reported for the individual patient.
Some private payers have instructed physicians to bill an office visit (99201-99215) based on the entire group visit. For compliance purposes, we recommend that you ask for these instructions in writing and keep them on file as you would any other advice from a payer.
Where each individual patient is provided a medically necessary, one-on-one encounter, in addition to the time in the group discussions, there should be no problem in billing for the visit based solely on the documented services provided in a direct one-on-one encounter.
If your group visits include the services of nutritionists or a behavioral health specialist, contact payers to determine if that portion of the group visit can be directly billed by the non-physician provider. This typically would include codes for medical nutrition therapy (97804) or health and behavior intervention (96153).
Other codes that may be applicable are the codes for education and training for patient self-management involving a standardized curriculum (98961-98962). Neither these codes nor medical nutrition or behavioral health therapy are billed by physicians. Physicians must use evaluation and management codes to report these services.
Code 99078 describes physician educational services in a group. Again, it is necessary to contact the payer to verify that coverage of this service is a payable benefit.
As with many services, coding for group visits requires that billing and coding staff do preliminary work with payers to identify desired coding applications.
Source: https://www.aafp.org/family-physician/practice-and-career/getting-paid/coding/group-visits.html
ARTICLE 2: “Telehealth Coding Guide”
There’s nothing more frustrating than rendering a service and not being paid. Nuanced coding rules are difficult to understand, and physicians aren’t taught this information in medical school.
Still, health care is a business. As business owners, physicians need to know how they’re paid, including what codes to use, what modifiers to append, and what details to document. Brushing up on common coding mistakes helps avoid costly recoupments and denials. We’ve asked several coding experts to provide their best advice on how physicians can maintain compliance and collect all of the revenue to which they’re entitled.
In part 1 of our two-part coding guide, we focused on coding for Telehealth and other forms of remote patient care — important codes for physician practices’ short-term survival as the U.S. continues to grapple with the COVID-19 pandemic.
Telephone services
In times of social distancing, telephone services have become a practical way to improve patient access and prevent the spread of COVID-19. Telephone services are ideal for straightforward problems (e.g., simple rash, asymptomatic cough, medication refills) that require a minimum of five minutes of medical discussion, says Toni Elhoms, CCS, CPC, chief executive officer of Alpha Coding Experts, LLC, in Orlando, Florida. Consider the following codes that Medicare accepts during the current public health emergency (PHE). Commercial payers may accept these codes, as well. Note that once the PHE has concluded, Medicare may only accept G2012 (virtual check-in) for telephone services.
Elhoms provides these tips to ensure compliance:
- Document verbal consent, including patient acknowledgment and acceptance of any copayments or coinsurance amounts due.
- Only count time spent on the phone engaging in medical discussion with the patient or caregiver. Do not report these codes for conversations lasting less than five minutes.
- Clearly document what was discussed, as well as the outcome of the conversation (e.g., medications prescribed, referrals to specialists, additional steps for the patient to take).
- Don’t report these codes when the telephone service ends with a decision to see the patient in 24 hours or the next available appointment.
- Don’t report these codes when the telephone service relates to a related E/M service performed within the previous seven days or within the postoperative period of a previously completed procedure.
- Only provide 99441-99443 and 98966-98968 for established patients. During the PHE, Medicare permits providers to bill G2012 for new and established patients.
‘The best way to operationalize these codes is to set up an edit in the practice management system that pends claims for a manual review to determine whether and which services are ultimately billable, Elhoms says.
Telehealth services
In the last few months, providers have adopted Telehealth to improve patient access and generate revenue during COVID-19. Among the services physicians can render via Telehealth to patients with Medicare during the current PHE are Medicare annual wellness visits, new and established patient office visits, prolonged services, smoking, and tobacco cessation counseling, annual depression and alcohol screenings, advanced care planning, and more. Medicare covers more than 200 services via Telehealth, many of which were added for temporary coverage during the current PHE. Commercial payer coverage of these services may vary, and it’s best to check with individual payers, Elhoms says.
Elhoms provides these tips for billing Telehealth services:
- Pay attention to audio-only vs. audio-visual requirements. Medicare requires the use of audio-visual technology for certain Telehealth services and permits audio-only for others. Commercial payers also may have specific requirements. For example, physicians can render a Telehealth visit for advanced care planning using audio-only, but they must use audio-visual technology for a new patient telehealth office visit.
- Don’t render Medicare’s Initial Preventive Physical Exam via Telehealth. Medicare does not permit it.
- Document verbal consent for Telehealth, including patient acceptance of any copayments or coinsurance amounts due.
- Use place of service (POS) code 11 and modifier -95 when billing Medicare. Note that commercial payers may require a different POS code (e.g., POS 2 or POS “other”) and modifier.
- Document, document, document. Physicians need to prove they met all of the code requirements even when rendering the service via Telehealth, Elhoms says. “Don’t pull in a problem list if you didn’t treat or manage all of those problems,” she adds. “Physicians need to link the diagnosis with the assessment and treatment plan. That’s imperative.” One caveat is that during the current PHE, physicians can bill 99201-99215 rendered via Telehealth based on time or medical decision-making. “The total time in direct medical discussion with the patient is going to be critical,” Elhoms says.
“The best advice I can give anyone doing Telehealth right now is to watch the CMS [Centers for Medicare & Medicaid Services] and commercial payer websites pretty much on a daily basis,” says Rhonda Buckholtz, CPC, CPMA, owner of Coding and Reimbursement Experts in Pittsburgh, Pennsylvania. “The coding of services changes constantly, and practices really need to be careful.”
Online digital E/M services
Though online digital E/M services are relatively new, they also can help practices increase patient access during COVID-19. Here’s how it works: An established patient initiates a conversation through a HIPAA-compliant secure platform (e.g., electronic health record portals, secure email, secure texting). A physician or other qualified health care professional reviews the query, as well as any pertinent data and records. Then they develop a management plan and subsequently communicate that plan to the patient or their caregiver through online, telephone, email or other digitally supported communication.
Elhoms provides these tips to maintain compliance:
- Use these codes when physicians or other qualified health care professionals make a clinical decision that would otherwise occur during an office visit. Do not use them for scheduling appointments or nonevaluative communication of test results.
- Use these codes only for established patients.
- Do not use these codes for fewer than five minutes of E/M services.
- Document verbal consent, including patient acknowledgment and acceptance of any copayments or coinsurance amounts due.
- Do not report these codes when the online digital E/M service ends with a decision to see the patient in 24 hours or the next available urgent visit appointment.
- Do not report these codes when the online digital E/M service relates to a related E/M service performed within the previous seven days or within the postoperative period of a previously completed procedure.
Promoting these services is often the biggest barrier, says Elhoms, who suggests putting up signs letting patients know they can access their provider electronically for non-urgent medical issues.
Remote patient monitoring
Remote patient monitoring (RPM) is a relatively easy way for physicians to keep tabs on patients without requiring them to come into the office. Medicare covers RPM for patients with one or more acute or chronic conditions, and commercial payer coverage may vary. During the PHE, physicians can initiate RPM on new and established patients. Normally, Medicare permits it only for established patients.
RPM consists of two forms: monitoring data through either a non-manual or manual data transfer, says Jim Collins, CPC, CCC, a consultant at CardiologyCoder.com, Inc. in Saratoga Springs, New York.
For example, physicians can remotely monitor a patient’s pulse oximetry, weight, blood pressure or respiratory flow rate using a device that transmits daily recordings or programmed alerts. Physicians can purchase them directly from manufacturers or patients can purchase the devices themselves. Collins says patients should look for Bluetooth-enabled devices or ones that include a built-in Global System for Mobile Communications (GSM) transmitter. The former requires an Internet connection, and the latter automatically transmits data to an internet cloud service through an encrypted bandwidth. Physicians can bill for the initial setup, cost of the device itself (when applicable), and data monitoring.
Another example is the self-measured blood pressure monitoring. When patients supply their own blood pressure device that a physician calibrates, physicians may be able to bill for patient education, device calibration, reviewing the data that the patient provides and communicating a treatment plan to the patient or caregiver.
“Monitoring physiologic data on a regular basis substantially reduces hospitalizations, trips to the emergency room and exacerbations of chronic conditions,” says Collins. “It can also be a huge chunk of revenue.”
Collins provides these tips for compliant RPM billing:
- Document patient consent. Patients must opt-in for these services.
- Document total time spent rendering these services to support time-based requirements.
- Know when these codes are appropriate. It’s unclear whether Medicare will pay physicians for monitoring physiologic data derived from internal devices (devices placed within the patient’s body) or data derived from wearable fitness devices.
- Only bill 99457 when the provider renders at least 20 minutes of live, interactive communication with the patient or caregiver. “It’s not going to be medically necessary to spend 20 minutes every month on every patient,” Collins says. “Patients could go for several months without physicians needing to do anything for them.”
Source: https://www.medicaleconomics.com/view/telehealth-coding-guide
“What’s Current in Coding?” is brought to you by EZClaim, a medical billing solution. To find out if it may work for you, either schedule a one-on-one consultation with their sales team, or download a FREE TRIAL to check it out the software yourself. For additional information right now, view their web site, send an e-mail to sales@ezclaim.com, or contact the sales team at 877.650.0904.

Sep 10, 2020 | Electronic Billing, Medical Billing Software Blog, Partner
In the wake of the COVID-19 pandemic, Telehealth adoption has exploded, and there are six revenue cycle metrics to track.
Many patients are prohibited or reluctant to venture out for on-site care. The combination of relaxed regulations and expanded payment parity for appointments has made virtual meetings easier and more attractive for providers, who are turning to these technologies to stay engaged with patients—and maintain cashflow. Dr. Robert McLean, a former president of the American College of Physicians, recently said, “this crisis has forced us to change how we deliver health care more in 20 days than we had in 20 years.”
A new industry report predicts that the number of Telehealth visits in the US will surpass one billion by the end of the year, and speculates that nearly half of those visits will be related to COVID-19. At Waystar, we have been closely monitoring claim trends and are seeing this growth firsthand. In fact, the volume of Telehealth claims on the Waystar platform has grown by more than 100 times since mid-March. On two particular days in late April, they accounted for more than 15% of our total daily claim volume. Before COVID-19, they would have accounted for less than one percent!
For many providers, this shift will require new revenue cycle strategies to meet growing patient demand without overwhelming clinicians and administrative teams—or already strained operating budgets. It’s important to remember this is still very much an evolving care delivery model with the opportunity for errors on the part of both payers, providers, and administrative staff. For this reason, revenue cycle professionals should diligently monitor claims to ensure proper adjudication, identify learning opportunities, and uncover areas for operational improvement.
Below, we’ve listed six core Telehealth-related metrics you should regularly track to ensure billing accuracy, maximize payer reimbursement, and reduce claim rejections and denials. For more on how to best navigate the evolving telemedicine landscape, check out our resource hub here.
To report on Telehealth-related claims, you’ll first need to identify and isolate claims containing Telehealth procedure codes. See CMS’ Telehealth code list to identify the specific procedure codes and modifiers that apply to your organization.
Payer Analysis:
1. Payer Telehealth claim rejections by volume and/or billed amount
2. Payer Telehealth claim denials by volume and/or billed amount
If your Telehealth claims are being denied or rejected, do you know which specific payers are doing so at the highest rate? Drill down to discover the specific reason codes payers are attaching to rejections and denials so you can better understand payer-specific rules and avoid these oversights in the future. In some cases, you may identify trends that warrant a call to the payer to correct.
Provider Analysis:
3. Telehealth claim volume by the provider
Review this claim volume by individual provider. If you notice providers within your organization generating a much lower volume of Telehealth claims than peers, perhaps they could benefit from additional training on Telehealth technology and use cases.
Ensuring Billing Accuracy:
4. Telehealth claim rejections by biller/team
5. Telehealth claim denials by biller/team
Are certain billing personnel or teams producing higher denial or rejection rates than others? Keep a close eye on these trends and remember most of this is new for everyone. If some team members are seeing more rejections or denials than they should, it could be a great opportunity to hold training and collaborate on strategies for success.
Maximizing Reimbursement:
6. Telehealth claim volume by procedure code
Which Telehealth codes are you using? Each code reimburses at a different rate, so choosing the wrong ones could leave money on the table. Be sure to read up on CMS’ requirements (check out their fact sheet and code list) to ensure you’re choosing the appropriate code(s) on each Telehealth claim.
Waystar Analytics
You have all the data you need to drive informed decision making and improve financial performance—you just need the right analytics tool in your corner. Our new Waystar Analytics solution offers a pre-built Telehealth dashboard that can help you easily interpret, share all the metrics above, and track these revenue cycle metrics. Click here to learn more about Waystar Analytics and how it can deliver the insights you need during this time of transition.
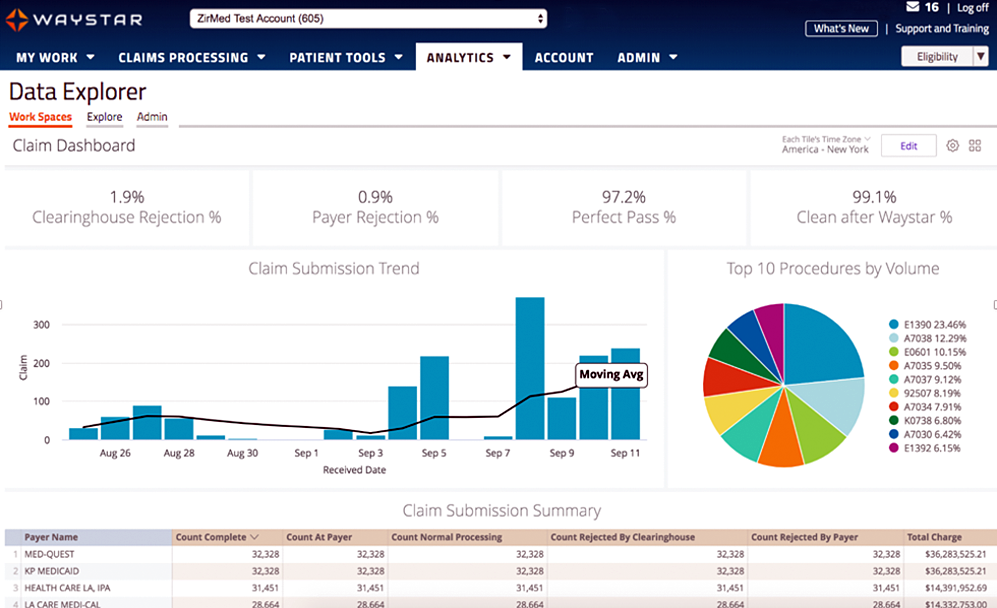
[ By Waystar ]

Jul 14, 2020 | BillFlash, NexTrust, Partner
The SIX KEYS to sustaining your practice through the COVID-19 pandemic are online payments, Telehealth, automation tools, cyber protection, financial aid, and a good patient experience.
When Coronavirus first started to impact medical practices across the country, providers quickly put temporary solutions in place to ensure they were still able to see patients safely. As the pandemic endured, some of these “temporary” solutions became a “normal” part of doing business. While we can’t predict exactly how COVID-19 will affect us in the future, one thing is becoming clearer every day: Some of the changes that have been made in the past few months will shape how healthcare is managed after the global health crisis is over.
So, it’s time to start thinking long-term with your COVID-19 strategy. Here are six ‘keys’ for sustaining your practice right now that will continue to be important after the pandemic is over.
1. ONLINE PAYMENTS
Most businesses already process a good amount of their payments online (including EZClaim), but healthcare has been slow to adapt in this area. Practices no longer have the luxury of taking their time adopting digital payment options. It’s time to give patients what they’ve been wanting for years: the ability to pay their bills online.
Because the pandemic is still with us, contactless payments have surged. No-touch payments are an easy way to reduce the spread of germs, and most people already have the tools they need to complete these types of payments: phones, computers, and credit cards.
Online payments are encouraged even when you’re meeting patients in the office. EZClaim customers can easily facilitate this with LinkPay. The process is easy and can be done once an appointment is made.
Here’s LinkPay in three simple steps:
1) Create a customized payment link with the required amount
2) Email or text the link to the patient before their visit
3) Patient pays the required amount, which is immediately confirmed and processed
COVID-19 demanded contactless payments for safety, but now patients now expect them for convenience. Medical practices will need online payments if they are to stay relevant in the future.
2. TELEHEALTH
Telehealth threw providers a lifeline when patients stopped coming into the office. The government acted quickly to relax Telehealth reimbursement policies so providers would be paid just as much for a Telehealth visit as they would for an in-office visit.
Congress is hoping to make these changes permanent. Whether they succeed or not, plan on keeping Telehealth as an option for your patients. Because Telehealth is not just useful during a pandemic, it’s great during normal life, too. Not all visits require an in-person encounter, and patients of all ages can benefit from the convenience of not having to physically leave their homes to get the medical care they need.
Patients have become used to having Telehealth as an option. Keeping it as an option going forward will set you apart from other practices.
3. AUTOMATION TOOLS
Chances are you are working with fewer people than normal. So, with fewer people to handle your billing and payments, your best option is to automate whatever you can.
This could mean setting up AutoPay for patients you see regularly, so they don’t have to manually pay their bill every time. It could also mean setting up a payment plan, in which a fixed amount will be paid automatically every month until the balance is paid off. It could also mean outsourcing your collections.
Automation doesn’t mean you lose control. Rather, it gives your staff more time to manage other essential operations. EZClaim customers have all of these automation options available to them through BillFlash.
4. CYBER PROTECTION
With digital tools becoming more prevalent, it is more important than ever to make sure your systems are protected. Hackers are out in full force right now, so it is imperative that you have proper malware and anti-virus software in place to protect your practice, your patients, and your employees. Do your homework on the tech companies you work with, too. Protecting your practice and your patients should be a top priority!
Of course, your staff will need to be up-to-date on HIPAA protocols, as well. Make sure you are doing everything you need to protect patient privacy online as well as offline.
5. FINANCIAL AID
Some practices are struggling financially and may need government aid to get them through the current crisis. Keep an eye on government funds that are available and stay informed on their different requirements.
If you haven’t already, consider applying for a line of credit. This is a standard operating procedure—even during normal times—and can help protect you from further financial disruptions in the future. No one knows how long this pandemic will last, so having a line of credit to fall back on during the coming months and years could be a game-changer for your practice.
6. A GOOD PATIENT EXPERIENCE
Above all, you need happy patients. That is true whether we are in a recession or not. Happy patients are more likely to pay their bills, more likely to return for future care, and more likely to recommend you to family and friends.
So, as you make some of the changes you made during the pandemic permanent, make sure you are still doing the little things to ensure a positive patient experience. These include:
• Keep wait times short
• Maintain eye contact during visits to assure patients that you care
• Be transparent about payment expectations and insurance, as well as what you’re doing to keep patients and staff safe
• Allow patients to pay using their preferred payment method
• Offer payment plans in lieu of paying large bills in one lump sum
A positive patient experience will be key in bringing your patients back to the office as the global health crisis continues.
NexTrust from BillFlash offers a variety of innovative billing and payments solutions for EZClaim customers. Visit billflash.com or e-mail them at Sales@BillFlash.com to learn more about how you can get paid more, get paid faster, and ensure you have the online tools you need to thrive during the pandemic.
For details and features about EZClaim’s medical billing software, or the other partners they have integrated into their billing solution, visit their website.
[ Written by Kathy Scott, Marketing Manager at BillFlash and NexTrust, Inc. ]







