
Jul 19, 2022 | EZClaim
Demand for different care models and emerging technologies are changing how healthcare is delivered in 2022. These are the trends to watch this year.
More Medical Technology Integration
Integrating medical technologies to broaden available data and improve patient outcomes will continue to impact the way hospitals, healthcare centers, and care providers operate. These new tools and integrations will allow healthcare professionals to use more efficient workflows thanks to better APIs and less data silos.
Integration means collecting more data with new remote monitoring and Medical “Internet of Things” devices. This data can then be centralized for patients and doctors with with cloud-based electronic health record platforms. It also means better patient education with consumer mobile apps, automated care-team emails and text messages, and digital therapeutics. These integrated tools will continue making it easier for doctors to collect and access more precise and detailed patient data than ever before.
As more technology works together, providers can identify and solve medical issues faster and more accurately. Further, patients are given opportunities to become more involved in achieving their healthcare goals and taking part in preventative measures.
Telehealth Continues to Grow
Today, many providers offer telehealth options to patients who prefer to meet with their doctor via phone or video. This option is one of the fastest growing in healthcare and will be an increasingly popular way to access healthcare in the coming years.
Telehealth can be beneficial for both providers and patients by lowering costs and increasing availability. Telemedicine allows healthcare providers to reduce their overhead and pass on those savings to patients by removing the need to visit a physical office. In addition, telehealth capabilities have made rural access easier by giving Americans a broader range of providers in different specialties. Traveling for healthcare can be expensive in terms of money and time. Virtual care offers lower costs, greater access to primary care for those in rural areas, and better public health.
The option to meet with a provider by phone or video is also a great tool to bring in and retain new patients. Lowering barriers to entry and establishing relationships via video or phone can be a great way to provide quality care initially and preserve that patient over the long term.
Healthcare consumerism was slowly growing before COVID, and patients see technology as a way to improve their mental and physical well-being. Telehealth will play a major role in those consumer expectations.
Home Health will Become More Popular
As more baby-boomers hit retirement age, demand for home health nurses and services—which were already seeing a surge in demand with COVID-19—will only continue to increase. As home health monitoring technology becomes increasingly available, states and private equity increases funding for these programs, and many seniors opt to return home instead of a skilled nursing facility, the trend towards home health is clear.
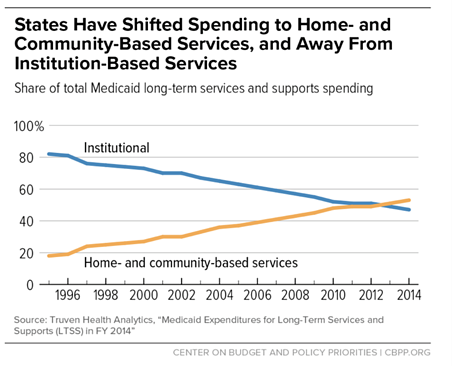
Medicare data reflects this trend as well with the Medicaid Innovation Accelerate Program reporting continued growth in home and community services.
Emerging technologies and care models are driving the way forward in 2022. These innovations will provide new ways for providers to deliver better care and more value to their patients.
EZClaim is a leading medical billing, scheduling, and payment software provider that combines a best-in-class product with exceptional service and support. For more information, schedule a consultation today, email our experts, or call at 877.650.0904.

Jul 12, 2022 | MedCycle Solutions, Partner
Have you increased the amount of Telehealth visits with your patients?
If not, you and your patients may be missing out.
Over the past two years, the COVID-19 pandemic has changed the landscape of patient care and increased the need for providers to utilize virtual healthcare services. Due to the Public Health Emergency (PHE) policy update, many healthcare practices had to shut down, pause or augment their services with telemedicine to provide flexibility in patient support.
Here are four ways Telehealthcare has been implemented to provide safe, necessary care for patients while augmenting revenue.
- Stop the Spread of Contagions
With the need to quarantine, social distance, and reduce the risk for clinic staff and patients, many health practices adapted ways of providing non-emergency services. For patients with (possible) highly contagious diseases, such as COVID-19, many clinics ask patients to schedule virtual appointments to avoid possible infections and further outbreaks. This allows for keeping both the staff and patients as safe as possible while still receiving necessary treatment.
- Provide Essential Health Services
For those patients that suffer from White Coat Syndrome going to the doctor’s office causes a great deal of stress and anxiety. By allowing patients to access care in the comfort of their own home for managing chronic health conditions, routine services, prescriptions, and referrals for testing and labs, this allows for greater patient access. Plus, it has the added benefit of reduced overhead costs associated with cleaning and turning exam rooms.
- Provide Physical and Occupational Therapy Healthcare
Accidents happen. Whether motor vehicle accidents, workplace injuries, or trips and falls – PT and OT is imperative to keep patients mobile and progressing. Many providers offer hybrid services with virtual appointments for patients to keep them mobile while supervising and adapting exercises in their home environments.
- Provide Mental and Behavioral Healthcare
Mental and behavioral healthcare is one of many patient-care needs. This is especially true for long-term residential care. Many nursing home facilities transitioned to telemedicine during the COVID-19 pandemic.
The U.S. Department of Health and Human Services, via the Centers for Medicare & Medicaid Services (CMS) heavily promoted the switch to Telehealth as infection prevention and control measures. They’ve made digital resources available that offer behavioral health and best practice guides for long-term nursing homes, a telemedicine tool kit, as well as other guidance.
If you think your practice and patients can benefit from implementing telehealth visits stay tuned for our next article on 5 Resources for Implementing Telehealth & Telemedicine.
Mariellen Mezzacappa has a variety of experience in the medical field. She has worked for doctors, hospitals, pharmacies, and insurance companies. Her experience includes bill review and coding with a wide range from EAPG 3M, DRG, Workers Compensation to Appeals and coder Affidavits for Litigation. She provides verification of code selection for operation reports, documentation review, and credentialing. Additionally, she has worked on operation policies, compliance training, and project management.
MedCycle Solutions provides Revenue Cycle Management, Credentialing, Outsourced Coding, and Consulting Services to a number of healthcare providers in a variety of specialties. To find out more about MedCycle Solutions services please visit www.MedCycleSolutions.com.

Jul 12, 2022 | Live Compliance, Partner
Whether you’re a one-person billing company or a multi-location organization, it’s possible that you’ve seen or heard of Malware and the potential risks associated with it and how it can cause major downtime and potential HIPAA violations due to breached information.
Criminals use malware to steal personal information, send spam, and commit fraud. Malware includes viruses, spyware, and other unwanted software that gets installed on your computer or mobile device without your consent. These programs can cause your device to crash and can be used to monitor and control your online activity. They also can make your computer vulnerable to viruses and deliver unwanted or inappropriate ads.
Here are a few, high-level quick steps you can take to spot and avoid Malware.
First, let’s talk security software.
Install and update security software, and use a firewall. Set your security software, internet browser, and operating system (like Windows or Mac OS X) to update automatically, and don’t forget to Back up your data regularly. Strong security software can prevent a hack or scam before it happens. You should install well-known software directly from the source. Sites that offer lots of different browsers, PDF readers, and other popular software for free are more likely to include malware. Read each screen when installing new software. If you don’t recognize a program or are prompted to install additional “bundled” software, decline the additional program or exit the installation process.
Don’t change your browser’s security settings and pay attention to your browser’s security warnings. Many browsers come with built-in security scanners that warn you before you visit an infected webpage or download a malicious file.
Next, watch what you’re clicking on.
Instead of clicking on a link in an email, type the URL of a trusted site directly into your browser. Scammers send emails that appear to be from companies you know and trust. The links may look legitimate, but clicking on them could download malware or send you to a scam site. Don’t open attachments in emails unless you know who sent it and what it is. Opening the wrong attachment — even if it seems to be from friends or family — can install malware on your computer.
Avoid clicking on pop-ups or banner ads about your computer’s performance! Scammers insert unwanted software into banner ads that look legitimate, especially ads about your computer’s health. Avoid clicking on these ads if you don’t know the source.
Your computer may be infected with malware if it:
-
- slows down, crashes or displays repeated error messages
- won’t shut down or restart
- serves a multitude of pop-ups
- serves inappropriate ads or ads that interfere with page content
- won’t let you remove unwanted software
- injects ads in places you typically wouldn’t see them, such as government websites
- displays web pages you didn’t intend to visit, or sends emails you didn’t write
Other warning signs of malware include:
-
- new and unexpected toolbars or icons in your browser or on your desktop
- unexpected changes in your browser, like using a new default search engine or displaying new tabs you didn’t open
- a sudden or repeated change in your computer’s internet home page
- a laptop battery that drains quicker than it should
At Live Compliance, we make checking off your compliance requirements extremely simple.
- Reliable and Effective Compliance
- Completely online, our role-based courses make training easy for remote or in-office employees.
- Contact-free, accurate Security Risk Assessments are conducted remotely. All devices are thoroughly analyzed regardless of location. Conducting an accurate and thorough Security Risk Assessment is not only required but is a useful tool to expose potential vulnerabilities, including those such as Password Protection.
- Policies and Procedures curated to fit your organization ensuring employees are updated on all Workstation Use and Security Safeguards in the office, or out. Update in real-time.
- Electronic, prepared document sending and signing to employees and business associates.
Don’t risk your company’s future, especially when we are offering a free Organization Assessment to help determine your company’s status. Call us at (980) 999-1585, or email me, Jim Johnson at Jim@LiveCompliance.com or visit www.LiveCompliance.com
For more information about DarkWeb breaches please contact us at (980) 999-1585 or email us at support@livecompliance.com

Jul 3, 2022 | Partner, Trizetto Partner Solutions
It’s safe to say that healthcare practitioners are well aware of the importance of credentialing. Beyond the legalities required of practicing physicians, credentials are needed for a practice’s revenue cycle to function properly. If providers aren’t enrolled with payers, they can’t receive payment for submitted claims. It’s as simple as that.
New and existing providers are required to maintain credentials and it’s not an easy process, even for the most well-oiled office. In order to take on the most patients and collect optimal revenue, practices also need to accept a wide array of payers. In fact, there has been a 5 percent uptick in providers enrolled with 10-20 payers, according to VerityStream’s 2018 Provider Enrollment Survey. Gaining enrollment with these payers involves verifying qualifications in order to accept patients, submit claims and ensure a steady stream of cash. Administrators need to collect the educational history of providers, fill out forms and submit the applications. It sounds easy enough, right?
Think again. There are hours of administrative work needed and a high risk for human error, with any hiccup in the process likely causing delays. It’s been said that up to 85% of credentialing applications are incomplete, which could cause delayed billing, lost revenue or even audits.
When it comes to credentialing, time is money. A 2016 survey by Merritt Hawkins found that a non-credentialed doctor was losing approximately $6,600 a day. Multiply that by the total amount of physicians in a given practice, and the potential losses are staggering.
Credentialing is a necessary evil, so do you handle in house or outsource? That’s the million dollar question. Utilizing current staff resources sounds like the easy solution, but does your organization have a dedicated employee to focus on your credentialing needs? Probably not. Chances are, this employee is pulled in many directions and isn’t able to dedicate time solely to credentialing. And if you do plan to handle the process with current staff, are your employees well-versed in all payers and their processes? Factor in learning curves or potential staff turnover and the time associated with training new employees and the not-so obvious financial costs quickly add up.
So how does the average practice streamline the process and ensure that credentials are gained as painlessly as possible? The old adage “you get what you pay for” could easily apply to this scenario. Hiring an outside resource means you are essentially paying for expertise and efficiency, which will save time and money in the long run. Why wouldn’t you want to utilize expert resources with in-depth knowledge of payer and state nuances? However, before making a decision, you need to know how much your practice could save by using a third party. Knowledge is power and having an accurate picture of your potential revenue is the first step to determining the best option for your organization.
Access the credentialing ROI calculator from TriZetto Provider Solutions, a Cognizant Company, to receive an estimate of potential revenue savings. Discover the hidden costs associated with the credentialing process and see just how much revenue your practice could be leaving on the table. You’ll gain enrollments quickly and accurately, keep employee satisfaction levels high (since they won’t be burdened by the process) and ultimately, increase revenue.
Don’t allow the complicated payer credentialing and enrollment process to be a burden on your practice. The credentialing experts at TriZetto Provider Solutions have experience working with various payers and providers of all backgrounds. Our team will collect and submit information in a timely manner and perform all necessary follow-up tasks. Let us lighten your load so you can focus on patient care and growing your practice.
[Contribution by TriZetto Provider Solutions Editorial Team]






