
Dec 14, 2020 | Live Compliance, Medical Billing Software Blog, Partner, Support and Training
There are a few HIPAA items to focus on RIGHT NOW—before the end of 2020!
The U.S. Department of Health and Human Services (HHS) has designated the “Health Insurance Portability and Accountability Act” (HIPAA) as the national standard for protecting the privacy and security of health information (in 1996). This led to the Health Information Technology for Economic and Clinical Health Act (HITECH), which has a provision in it for audits, and the HHS Office for Civil Rights is responsible for carrying out HIPAA audits, and responding to complaints and breaches. Ignoring them is not an option!
A Risk Assessment IS NOT Enough
A risk assessment is only one element of the compliance process. You must also “implement security updates as necessary and correct identified security deficiencies.” In other words, you must act via a Corrective Action Plan (CAP) and follow the required risk assessment process.
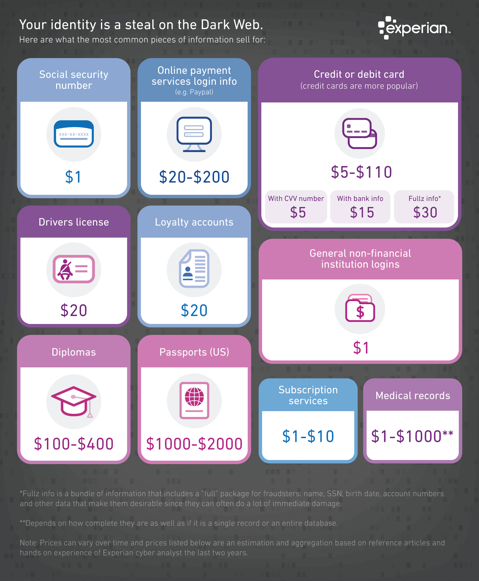
Dark Web
It is no secret that the “Dark Web” is a scary place to lose your information. So, what if it did happen and affected your entire company? Identity thieves get anywhere from $1-$1,000 for medical records, for each instance! So, how can you protect yourself and/or your organization?
Well, data breaches are becoming more common—sometimes which are out of your control—so carefully monitoring where you store and enter your passwords can be extremely beneficial to help minimize the risk of a hack and keeping personal or patient information protected.
One solution for this is the automatic Dark Web monitoring built into the portal of one of EZClaim’s partners, Live Compliance. Their solution helps keep an ‘eye’ on employees whose information was involved in a breach, and suggests next steps to take where the breach was found. Then, it allows your to conduct an accurate and thorough Security Risk Assessment. This is not only required, but is a useful tool to expose potential vulnerabilities, including those that involve password protection.
 So, what can I do to ensure this doesn’t happen to me or my organization? Well, Live Compliance makes checking off your compliance requirements extremely simple by providing:
So, what can I do to ensure this doesn’t happen to me or my organization? Well, Live Compliance makes checking off your compliance requirements extremely simple by providing:
● Reliable and effective compliance
● Completely online, our role-based courses make training easy for remote or in-office employees
● Contact-free, accurate Security Risk Assessments are conducted remotely. All devices are thoroughly analyzed regardless of location.
● Policies and procedures are curated to fit your organization, ensuring employees are updated on all workstation use and security safeguards in the office, or out. It is updated in real time.
● An electronic document is sent to employees and business associates
So, don’t risk your company’s future, especially when Live Compliance offers a FREE Organization Assessment to help determine your company’s status.
For additional details, call them at 980.999.1585, e-mail them, or visit their website at LiveCompliance.com
[ Article provided by Jim Johnson of Live Compliance ].
ABOUT EZCLAIM:
EZClaim is a medical billing and scheduling software company that provides a best-in-class product, with correspondingly exceptional service and support. Combined, they help improve medical billing revenues. To learn more, visit EZClaim’s website, e-mail them, or call a representative today at 877.650.0904.

Oct 12, 2020 | Electronic Billing, Features, Medical Billing Software Blog
EZClaim Launches EZClaimPay, a new feature in its medical billing software that makes credit card processing painless!
EZClaim, a company with the mission of elevating its clients to stay in front of the ever-changing landscape of medical billing, announced today the launch of its credit card processing feature and service called, EZClaimPay.
EZClaim released the product in August 2020 as a solution to the ever-changing landscape of payment reconciliation. It was cited by customers as a timely response to a ‘pain point’—credit card payment processing—another example of EZClaim’s devotion to their mission.
Dan Loch, VP of Marketing commented that “EZClaim’s goal continues to be making life easier for medical billers at practices and billing firms. EZClaimPay is just one more feature within our mission of living up to that goal.” This feature will help companies get in front of the changes in medical transparency that are coming soon.
EZClaimPay provides for consolidated reconciliation (Payment reports; Chargeback management; and Reconciliation reports) and a single point of contact for support (Hardware; Software; and Payments).
EZClaim has developed a robust payments platform—tightly integrated with their software and support—to make accepting credit cards for payment PAINLESS! EZClaimPay makes software and payments better together.
For more details about EZClaimPay, view this web page: https://ezclaim.com/ezclaimpay/
ABOUT EZCLAIM:
EZClaim is a medical billing and scheduling software company that provides best-in-class customer service and support. To learn more, e-mail them at sales@ezclaim.com or call a representative today at 877.650.0904.

Sep 10, 2020 | Electronic Billing, Medical Billing Software Blog
So, it looks that there will be a lot new for E/M coding (Evaluation and Management) in 2021, and practices should start to get ready for it.
Well, it seems the only constant in the world of medical billing changes, and 2020 would only compliment that cliché. While the chaos of COVID-19 forced many unexpected changes—how you see your patients and bill for services—a bigger change is in the works for 2021. This change will complement the “Patients Over Paperwork” initiative from CMS and the AMA, which has been developed to eliminate “Note Bloat.” So, since the new year will roll out changes to E/M visits, now is the time to make sure that all parties are prepared for this long overdue and welcome change to medical billing.
Evaluation and management services have been long overdue for an overhaul. The 1995/1997 guidelines were in place well before electronic medical records, and with the growth of EMR’s, the process to document for a specific level required a lot of tedious, unnecessary documentation. (A cursory look at some of the proposed updates for E/M CPT coding and documentation requirements will verify that!)
PROPOSED CHANGES:
• History and Examination: While the elements of history and examination that are pertinent to a specific visit shall be recorded, they will no longer be used to ‘score’ the level billed
• Code Selection: It will be based on MDM or time
• Medical Decision Making: It will still utilize the CMS Table of Risk. However, the wording and explanations are being updated to provide more concise language. For instance, definitions will now be included to clearly identify subjective wording like “self-limited and stable chronic illness.” The clinical example will likely be removed, and the terms are more clearly defined. We will see this same type of clarification in the MDM table. For example, the 2021 guidelines will specify that the amount and/or complexity of data to be reviewed must also include analysis.
• Time-based Code Selection: It will also be easier. The guidelines will give specific amounts of time rather than the generic estimate that we currently see attached to E/M codes. Another major advantage to the codes selected based on time, they will now include non-face-to-face services. There will also be additional add on codes—in 15-minute increments—if the time has been exceeded for the 99205 or 99215.
While changes are daunting, this change will be rewarding from a documentation standpoint. So, if you need help with training your team on these new updates, there are FREE videos available on the AMA website, or you can enlist the help of an independent consultant like RCM Insight.
One way of keeping up with these changes is to use EZClaim’s medical billing software, which is continually updated. For more details, visit their website, ezclaim.com, contact them, or just give them a call at 877.650.0904.
[ Written by Stephanie Cremeans of EZClaim ]

Aug 11, 2020 | ChartSwap, Partner
An online “Health Information Exchange” (HEI) can be the answer to managing the release-of-information (ROI) process completely digitally.
Many healthcare providers are spending a significant amount of time and money on fulfilling requests for medical and/or billing records. Outdated and inefficient modes of technology like printers, postal mail and fax machines make up much of that cost. Time spent on having employees complete record fulfillment operation—or money spent on working with third-party release-of-information (ROI) companies—add significantly to strains on manpower and/or budgets. Then add in the money spent on postage and in-office time spent responding to status calls, and you have a significant cost center that is not benefitting your business.
In today’s digital world, both businesses and consumers expect efficient, safe, online transactions. While the healthcare industry had a longer grace period for digital transformation initiatives, a new survey reveals that 75% of people now expect the same service from healthcare organizations that they receive from other businesses. This is driving many organizations to re-think the current, highly ROI process and seek a simple, secure, and more cost-effective digital ROI solution.
Utilizing an online Health Information Exchange may be the answer to your problems. By utilizing the FREE proprietary software that the country’s fastest growing HIE, ChartSwap, healthcare entities can manage the ROI process completely digitally in a HIPPA- and HITECH-compliant, SOC 2, Type II-certified and conveniently cloud-based environment. In addition to eliminating the need for paper, printers, postage, and other unnecessary and inconvenient expenses, ChartSwap allows records providers to conduct all communication with requestors 100% online without the security concerns associated with e-mail.
ChartSwap users set their own fees and can quickly and conveniently collect payments electronically via either credit card or PayPal (which includes the option for ACH transfer). Over 90% of ChartSwap requestors use online payment methods, and for the few who still prefer to send a paper check, ChartSwap handles the receipt and processing of those payments on your behalf. That means that 100% of your payments for medical and billing records will be handled by the ChartSwap platform—at absolutely no cost to you!
Using ChartSwap has been shown to improve employee productivity by 50% or more, thanks to ChartSwap’s advanced digital workflows, automatic status alerts, and fully online communication model. Additionally, the turnaround time for fulfilling records requests via ChartSwap can be as quick as two days and rarely exceeds 14 days—that’s more than 50% faster than the turnaround time on requests fulfilled by traditional methods.
To learn more about taking back control of your office’s record fulfillment operations, and turn this cost center into a profit center, visit ChartSwap today.
ChartSwap is a partner of EZClaim, a medical billing software solution. For more details about EZClaim, visit their website at EZClaim.com

 So, what can I do to ensure this doesn’t happen to me or my organization? Well, Live Compliance makes checking off your compliance requirements extremely simple by providing:
So, what can I do to ensure this doesn’t happen to me or my organization? Well, Live Compliance makes checking off your compliance requirements extremely simple by providing:



